New research study shows COVID-19 antibodies continue a minimum of 9 months after infection.
Testing of a whole Italian town reveals antibody levels stay high 9 months after SARS-CoV-2 infection, whether symptomatic or asymptomatic.
Researchers from the University of Padua and Imperial College London evaluated more than 85 percent of the 3,000 citizens of Vo’, Italy, in February/March 2020 for infection with SARS-CoV-2, the infection that triggers COVID-19, and evaluated them once again in May and November 2020 for antibodies versus the infection.
The group discovered that 98.8 percent of individuals contaminated in February/March revealed noticeable levels of antibodies in November, and there was no distinction in between individuals who had actually suffered signs of COVID-19 and those that had actually been symptom-free. The outcomes are released today (July 19, 2021) in Nature Communications.
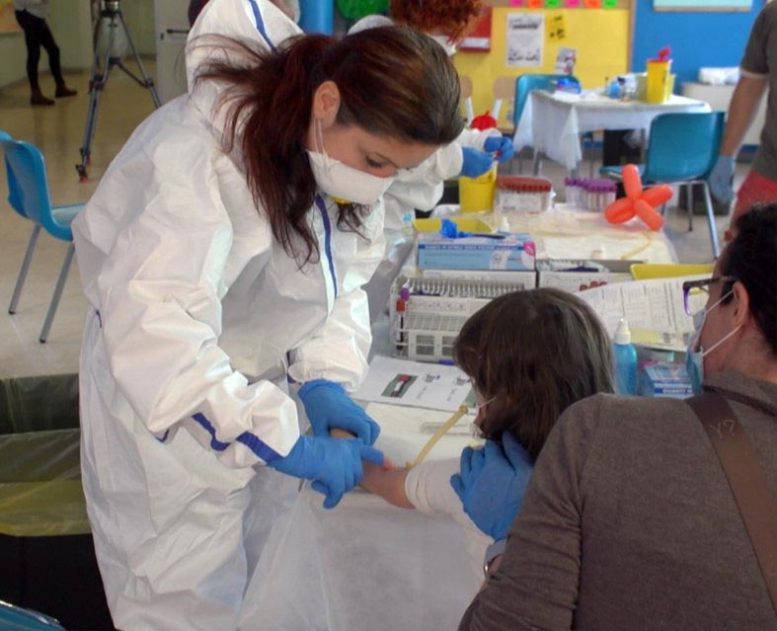
A scientist screening a kid as part of the research study. Credit: Andrea Crisanti
Antibody levels were tracked utilizing 3 ‘assays’ – tests that find various kinds of antibodies that react to various parts of the infection. The results revealed that while all antibody types revealed some decrease in between May and November, the rate of decay was various depending upon the assay.
The group likewise discovered cases of antibody levels increasing in some individuals, recommending prospective re-infections with the infection, offering an increase to the body immune system.
Lead author Dr Ilaria Dorigatti, from the MRC Centre for Global Infectious Disease Analysis and the Abdul Latif Jameel Institute for Disease and Emergency Analytics (J-IDEA) at Imperial, stated: “We discovered no proof that antibody levels in between symptomatic and asymptomatic infections vary considerably, recommending that the strength of the immune action does not depend upon the signs and the intensity of the infection.
“However, our study does shows that antibody levels vary, sometimes markedly, depending on the test used. This means that caution is needed when comparing estimates of infection levels in a population obtained in different parts of the world with different tests and at different times.”
Professor Enrico Lavezzo, from the University of Padua, stated: “The May screening showed that 3.5 percent of the Vo’ population had actually been exposed to the infection, although not all of these topics knew their direct exposure provided the big portion of asymptomatic infections.
“However, at the follow-up, which was performed roughly nine months after the outbreak, we found that antibodies were less abundant, so we need to continue to monitor antibody persistence for longer time spans.”
The group likewise examined the infection status of family members, to approximate how most likely a contaminated member is to hand down the infection within the family. Their modeling recommends that there was a likelihood of about 1 in 4 that an individual contaminated with SARS-CoV-2 passes the infection to a relative which the majority of transmission (79 percent) is triggered by 20 percent of infections.
This finding validates that there are big distinctions in the variety of secondary cases created by contaminated individuals, with most of infections producing no additional infections and a minority of the infections producing a a great deal of infections.
The big distinctions in how one contaminated individual might contaminate others in the population recommends that behavioral aspects are essential for epidemic control, and physical distancing, along with restricting the variety of contacts and mask using, continue to be necessary to minimize the danger of transferring the illness, even in extremely immunized populations.
The group’s dataset, that includes the outcomes of the 2 mass PCR screening projects carried out in February and March and the antibody study carried out in May and after that once again in November, likewise permitted them to tease apart the effect of numerous control steps.
They revealed that, in the lack of case seclusion and brief lockdowns, manual contact tracing alone would not have actually sufficed to reduce the epidemic.
Project lead Professor Andrea Crisanti, from the Department of Life Sciences at Imperial and the Department of Molecular Medicine at the University of Padua, stated: “Our study also shows that manual contact tracing – the search for positive individuals on the basis of known and declared contacts – would have had a limited impact on the containment of the epidemic, had it not been accompanied by a mass screening.”
Dr. Dorigatti included: “It is clear that the epidemic is not over, neither in Italy nor abroad. Moving forward, I think that it is of fundamental importance to continue administering first and second vaccine doses as well as to strengthen surveillance including contact tracing. Encouraging caution and limiting the risk of acquiring SARS-CoV-2 will continue to be essential.”
Reference: “SARS-CoV-2 antibody dynamics and transmission from community-wide serological testing in the Italian municipality of Vo’” by Ilaria Dorigatti, Enrico Lavezzo, Laura Manuto, Constanze Ciavarella, Monia Pacenti, Caterina Boldrin, Margherita Cattai, Francesca Saluzzo, Elisa Franchin, Claudia Del Vecchio, Federico Caldart, Gioele Castelli, Michele Nicoletti, Eleonora Nieddu, Elisa Salvadoretti, Beatrice Labella, Ludovico Fava, Simone Guglielmo, Mariateresa Fascina, Marco Grazioli, Gualtiero Alvisi, Maria Cristina Vanuzzo, Tiziano Zupo, Reginetta Calandrin, Vittoria Lisi, Lucia Rossi, Ignazio Castagliuolo, Stefano Merigliano, H. Juliette T. Unwin, Mario Plebani, Andrea Padoan, Alessandra R. Brazzale, Stefano Toppo, Neil M. Ferguson, Christl A. Donnelly and Andrea Crisanti, 19 July 2021, Nature Communications.
DOI: 10.1038/s41467-021-24622-7