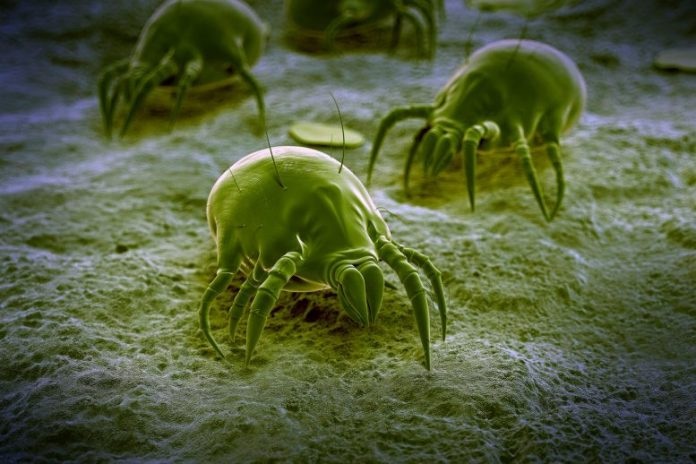
These tiny animals are difficult to prevent, which suggests almost everybody has actually been exposed.
Study opens brand-new course to research study to combating allergic illness.
The world has lots of home allergen. Do some cleansing, and you’ll most likely stir some up. While everybody has immune cells efficient in responding to typical irritants like home allergen, the majority of us have no allergic signs.
Still, lots of people do respond with the normal allergic signs: sneezing, a runny nose, and scratchy, inflamed nasal passages. Others have a a lot more extreme response: a lethal asthma attack.
To deal with the origin of allergic reactions and asthma, scientists require to understand precisely what sets these clients apart from healthy people.
In a brand-new Science Immunology research study, released on June 12, 2020, researchers at La Jolla Institute for Immunology (LJI) use a hint to why non-allergic individuals don’t have a strong response to house allergen. They’ve revealed a formerly unidentified subset of T cells that might manage allergic immune responses and asthma from ever establishing in action to house allergen — and other possible irritants.
“We discovered new immune cell subsets and new therapeutic opportunities,” states Grégory Seumois, Ph.D., trainer and director of LJI’s Sequencing Core and co-leader of the brand-new research study. “This new population of cells could be one, out of many unknown mechanisms, that explains why healthy people don’t develop inflammation when they breathe in allergens.”
“The study highlights the power of unbiased single-cell genomics approaches to uncover novel biology,” states LJI Professor Pandurangan Vijayanand, M.D. Ph.D., senior author of the brand-new research study.
The research study constructs on the Vijayanand laboratory’s competence in connecting gene expression to illness advancement. The group likewise benefited from the Immune Epitope Database, an LJI-led resource that houses info on how the body immune system engages with irritants like home allergen.
Why home allergen? These tiny animals are difficult to prevent, which suggests almost everybody has actually been exposed. Even in individuals without a home allergen (HDM) allergic reaction, the body immune system is most likely to respond in some method as it discovers to acknowledge HDM particles. This makes HDM a useful design for studying what triggers allergic reactions and asthma attacks.
The LJI group utilized a strategy part of the “genomic revolution” toolbox of tools, called single-cell RNA-seq (or single cell transcriptomics) to see precisely which genes and particles particular T cells produce in action to HDM irritants. They checked cells from 4 groups of individuals: individuals with asthma and HDM allergic reaction, individuals with asthma however no HDM allergic reaction, individuals with just HDM allergic reaction, and healthy topics.
Their analysis recommends that a subset of assistant T cells, called interleukin (IL)-9 Th2 revealing HDM-reactive cells, is more widespread in the blood of individuals with HDM-allergic asthma compared to those who are just adverse HDM. Further analysis recommended that those IL9-TH2 cells are improved in a group of molecules/genes that increased the cytotoxic capacity of those cells. In other words, those particular T cells might eliminate other cells and drive swelling.
In contrast, another subset of T cells stood apart in the non-allergic topics. These T cells reveal an “interferon response signature” and were improved for a gene that encodes a protein called PATH. The work done by Seumois and his coworkers recommend that PATH might be crucial since it might moisten the activation of assistant T cells.
This finding might suggest that individuals with this particular cell population might have less T-cell driven swelling in action to HDM irritants. At last, this might supply a hint to why some individuals establish allergic reactions and asthma while others do not.
“Now if functional studies confirm this dampening effect, we’re curious if there is a way to boost the activation of these T cells or induce their proliferation in asthmatic or allergic populations,” states Seumois. “Can we act on those cells very early on, before asthma has developed?”
For example, genomics research studies like this one might at some point assist recognize kids at threat of establishing asthma and allergic reactions. Early detection might unlock to preemptively acting upon immune cells prior to advancement of allergic reaction and asthma.
While Seumois stresses that there is far more work to be done, he states the transcriptomic technique utilized for this research study might speed up future asthma and allergic reaction research study. “This is the first large-scale, single-cell, RNA-seq transcriptomic analysis for LJI,” states Seumois. “Now that we have developed the bench know-how and analysis pipeline, it could be applied to many diseases.”
###
Reference: “Single-cell transcriptomic analysis of allergen-specific T cells in allergy and asthma” by Grégory Seumois, Ciro Ramírez-Suástegui, Benjamin J. Schmiedel, Shu Liang, Bjoern Peters, Alessandro Sette and Pandurangan Vijayanand, 12 June 2020, Science Immunology.
DOI: 10.1126/sciimmunol.aba6087
The research study, entitled “Single-cell transcriptomic analysis of allergen-specific T cells in allergy and asthma,” was supported by the National Institutes of Health (grants U19AI100275, U19AI135731, R01HL114093, S10RR027366 and S10 RR027366) and the William K. Bowes Jr. Foundation
Additional research study authors consisted of Ciro Ramírez-Suástegui, Benjamin J. Schmiedel, Shu Liang, Bjoern Peters and Alessandro Sette.