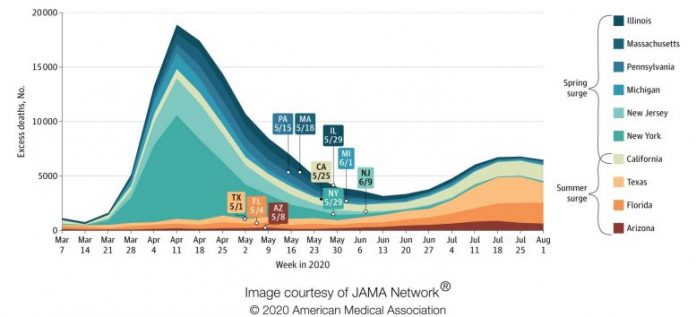
This chart reveals the variety of weekly excess deaths for the 10 specifies with the biggest variety of excess deaths throughout March-July 2020. The dates on the chart show when broad COVID-19 limitations were raised in each state utilizing information from reports by The New York Times. Credit: Courtesy of JAMA Network
States that resumed quicker, such as Texas, Arizona and Florida, experienced summer season rises, report states.
For every 2 deaths credited to COVID-19 in the U.S., a 3rd American passes away as an outcome of the pandemic, according to brand-new information publishing today (October 12, 2020) in the Journal of the American Medical Association.
The research study, led by scientists at Virginia Commonwealth University, reveals that deaths in between March 1 and Aug. 1 increased 20% compared to previous years — perhaps not unexpected in a pandemic. But deaths credited to COVID-19 just represented 67% of those deaths.
“Contrary to skeptics who claim that COVID-19 deaths are fake or that the numbers are much smaller than we hear on the news, our research and many other studies on the same subject show quite the opposite,” stated lead author Steven Woolf, M.D., director emeritus of VCU’s Center on Society and Health.
The research study likewise includes suggestive proof that state policies on resuming early in April and May might have sustained the rises experienced in June and July.
“The high death counts in Sun Belt states show us the grave consequences of how some states responded to the pandemic and sound the alarm not to repeat this mistake going forward,” stated Woolf, a teacher in the Department of Family Medicine and Population Health at the VCU School of Medicine.
Total death counts in the U.S. are extremely constant from year to year, as the research study notes. The research study authors pulled information from the Centers for Disease Control and Prevention for 2014 to 2020, utilizing regression designs to anticipate anticipated deaths for 2020.
The space in between reported COVID-19 deaths and all unforeseen deaths can be partly discussed by hold-ups in reporting COVID-19 deaths, miscoding or other information restrictions, Woolf stated. But the pandemic’s other causal sequences might describe more.
“Some people who never had the virus may have died because of disruptions caused by the pandemic,” stated Woolf, VCU’s C. Kenneth and Dianne Wright Distinguished Chair in Population Health and Health Equity. “These include people with acute emergencies, chronic diseases like diabetes that were not properly care for, or emotional crises that led to overdoses or suicides.”
For example, the research study particularly revealed that the whole country experienced considerable boosts in deaths from dementia and cardiovascular disease. Woolf stated deaths from Alzheimer’s illness and dementia increased not just in March and April, when the pandemic started, however once again in June and July when the COVID-19 rise in the Sun Belt took place.
This research study, with information from March to August 1, develops on a formerly released JAMA short article by the exact same authors from VCU and Yale University that concentrated on information from March to May 1. And it generates brand-new information about the timing of when states raised limitations on social distancing.
States like New York and New Jersey, which were struck hard early, had the ability to flex the curve and bring death rates down in less than 10 weeks. Meanwhile, states such as Texas, Florida and Arizona that got away the pandemic initially however resumed early revealed a lengthy summer season rise that lasted 16-17 weeks — and was still underway when the research study ended.
“We can’t prove causally that the early reopening of those states led to the summer surges. But it seems quite likely,” stated Woolf. “And most models predict our country will have more excess deaths if states don’t take more assertive approaches in dealing with community spread. The enforcement of mask mandates and social distancing is really important if we are to avoid these surges and major loss of life.”
Woolf paints a grim image, alerting that long-lasting information might reveal a more comprehensive effect of the pandemic on death rates. Cancer clients who have actually had their chemotherapy interrupted, ladies who have actually had their mammograms postponed — avoidable, sudden deaths might increase in the coming years, he stated.
“And death is only one measure of health,” Woolf stated. “Many people who survive this pandemic will live with lifelong chronic disease complications. Imagine someone who developed the warning signs of a stroke but was scared to call 9-1-1 for fear of getting the virus. That person may end up with a stroke that leaves them with permanent neurological deficits for the rest of their life.”
Diabetes problems that aren’t being handled appropriately might cause kidney failure and dialysis. And behavioral health problems, like psychological injury, are going without treatment. Woolf stresses most about the long lasting results on kids — long-lasting, generational results.
“This isn’t a pandemic involving a single virus,” stated Peter Buckley, M.D., dean of the VCU School of Medicine. “This is a public health crisis with broad and lasting ripple effects. VCU researchers have been diligent in their investigations into both treatment of COVID-19 and in understanding the long-term repercussions of the pandemic, so that fellow doctors, policymakers and community members can fight these battles on multiple fronts.”
Co-authors on Woolf’s paper consist of: Derek Chapman, Ph.D., Latoya Hill, DaShaunda Taylor and Roy Sabo, Ph.D., of VCU; and Daniel Weinberger, Ph.D., of Yale University.
The research study matches another VCU scientist’s current information revealing a disconcerting rise in opioid overdoses at VCU Medical Center throughout the pandemic. Taylor Ochalek, Ph.D., a postdoctoral research study fellow at the Wright Center, discovered a 123% boost in nonfatal overdoses in between March and June this year, as compared to last, in a research study likewise released in JAMA.
Woolf keeps in mind that the CDC has actually launched provisionary overdose deaths under a broad label called “external causes,” which likewise consists of auto accident and murders, making research study like Ochalek’s even more essential.
“Car crashes decreased because fewer people were driving during the lockdowns,” Woolf stated. “We worry that the broad umbrella category of ‘external causes’ may hide an increase in deaths from overdoses, because the opioid epidemic didn’t go away.”
The CDC, Woolf included, has actually hurried out provisionary death information this year since of the pandemic. More trustworthy, granular information will come out later on and enable scientists to unload the in-depth factors to excess deaths and secondary health effects of the pandemic.
Researchers throughout numerous disciplines at VCU are studying the secondary health effects of the pandemic — from compound usage conditions and intimate partner violence to reduced access to routine healthcare — all of which might add to death, according to Woolf’s research study.
Reference: 12 October 2020, JAMA.
DOI: 10.1001/jama.2020.19545