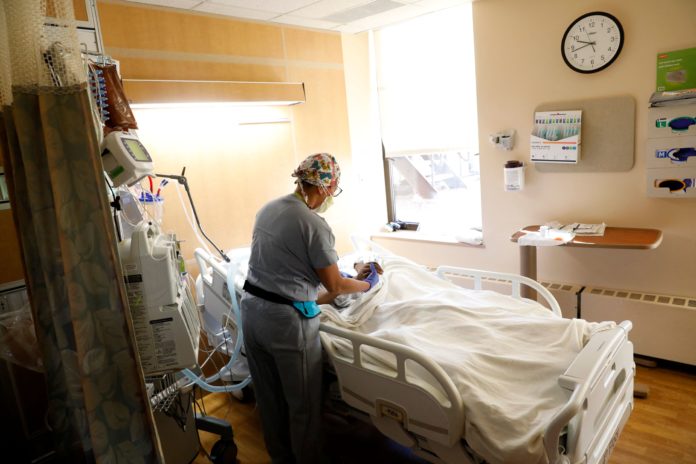
United States Army Critical Care Nurse, Captain Catherine Sison, tends to a non-covid client on a ventilator at Beaumont Hospital in Dearborn, Michigan, on December 17, 2021.
Jeff Kowalsky|AFP|Getty Images
Hospitals throughout the nation are bracing for another wave of Covid-19 cases that assures to be simply as bad, if not even worse, than the early days of the pandemic.
But this time, they are facing it with less nurses; and the personnel that stays is tired after practically 2 years of combatingCovid The health-care market lost 450,000 employees from February 2020 through November, primarily nurses and residential-care staff members, the Bureau of Labor Statistics reported previously this month.
What’s more, the extremely altered and infectious omicron version can more quickly contaminate immunized staff members than previous pressures. That threatens to additional intensify the staffing lack by sending out employees house to separate, even if they have moderate or no signs.
Retaining sufficient employees isDr Shereef Elnahal’s “biggest concern right now by far,” he stated. At the University Hospital in Newark, New Jersey, where Elnahal is president and CEO, the variety of staff members out of work due to Covid has actually doubled for the last 3 successive weeks in a row, he stated in a phone interview.
“It’s a concern that actually exceeds my concern over omicron-specific hospital admissions based on the trends that we’re seeing,” he stated.
Isolation
While the health center’s had the ability to discover individuals to fill those shifts today, “if that trend continues we will be in a very difficult position and we will have to move into crisis staffing,” he stated.
One of the primary factors health systems like his have actually mandated vaccines for employees was to keep them healthy so they might continue looking after ill clients. Omicron, nevertheless, provides a difficulty due to the fact that it appears to contaminate totally immunized individuals. Even asymptomatic cases need a minimum of 7 days of seclusion for health employees under standards from the Centers for Disease Control and Prevention.
“But if they end up getting Covid without symptoms and they still have to be out, that ends up, on the other end, posing a health-care risk and a quality risk to our patients,” Elnahal stated.
At South Dakota- headquartered Sanford Health, health center authorities are seeing Covid cases surge in other parts of the nation and changing their own rise strategies.
Preparing
“We’re taking this time to step back and prepare,” stated Erica DeBoer, primary nursing officer atSanford “What worked about our surge plan before and how do we fine-tune that so that we’re well prepared?”
For Sanford, that consists of drawing from a main labor force it’s formed to guarantee additional assistance at especially hectic times. The swimming pool includes more than 700 individuals throughout the system who get extra training and versatility with their present functions to assist fill out the spaces. That consists of both scientific and nonclinical personnel, who can aid with particular nursing work that does not need a license to provide nurses a break or let them concentrate on more pushing requirements.
Ohio- based Bon Secours Mercy Health sped up execution of a brand-new scheduling system throughout the pandemic so employees might reserve additional shifts ahead of time and have more certainty over their schedules, Dani Bowie, vice president of nursing labor force advancement, stated.
Traveling nurses firm Trusted Health is currently seeing a rise in need for employees comparable to previous waves at approximately 4 times greater than typical, according to Amanda Maxedon, vice president of market.
Mental health effect
Health employees at the start of the pandemic likewise weren’t fighting with practically 2 years of tiredness.
“The real problem is everybody’s tired,” stated Betty Jo Rocchio, primary nursing officer at Mercy, a system operating in numerous states consisting of Missouri andOklahoma “Everybody is mentally, physically and emotionally worn out from dealing with the impact of Covid.”
Rocchio stated Mercy provides a staff member help program with psychological health developed into it and the system likewise gets in touch with more unlicensed employees to assist cover particular jobs to help clients. She stated they have actually made a “conscious shift” to discover extra personnel and train them up.
“I think that’s a big de-stresser, knowing there’s more help coming on the units than there has been in the past,” she stated.
Trauma and fatigue
While health-care systems take actions to support their employees’ psychological health, Maxedon stated it is necessary for the assistance to feel significant to staff members. Providing treatment and area for employees to talk through their experiences throughout the pandemic are the kinds of things that “go a lot farther” than pizza celebrations and one-off yoga classes, she stated.
“I think the trauma that the nurses are going through is going to be a bit deeper than that, and so having long-term sustainable programs is going to be really important,” she included.
While incomes for taking a trip nurses have actually increased throughout the pandemic and normally double throughout rises, the additional pay alone isn’t reward enough for some.
“In 2019, it was hopeful that it was going to be short-lived and nurses were really flocking to help and wanting to help. And what we’re seeing this time around is I think nurses are more frustrated and they’re tired and they’re burnt out,” Maxedon stated. “And so while the pay may be increasing, it’s not enough anymore to get nurses to take those roles.”
Subscribe to CNBC on YouTube.
VIEW: The CDC anticipates in between 600,000 and 1.3 million brand-new Covid cases by Christmas