An affordable ventilator. Credit: Mohamed Amine Abassi
Researchers are establishing easy and affordable tools — like a Do It Yourself ventilator — to deal with clients better and avoid illness transmission in health centers.
The quick spread of COVID-19 overwhelmed health centers that were not able to compete with the increasing variety of clients, lots of needing ventilators and other vital care. Such conditions can put medical employees at danger. Now scientists are studying approaches to increase healthcare facility security and effectiveness throughout the pandemic.
A scarcity of life-saving ventilators, which generally cost around $30,000 each, struck health centers especially hard.
“By building a simple and cheap ventilator, we can help alleviate this burden for the medical staff,” stated Mohamed Amine Abassi, a PhD trainee in fluid mechanics.
Based on a model created by his consultant, engineering teacher Xiaofeng Liu, Abassi led an effort with coworkers from San Diego State University and the University of California San Diego to construct such a gadget from easily offered parts — plastic tubing, pressure valves, humidifier — and an air supply. Then they evaluated it.
Preliminary results shared at the 73rd Annual Meeting of the American Physical Society’s Division of Fluid Dynamics recommend the ventilator fulfills vital requirements set by the Food and Drug Administration. It is completely manageable on 3 criteria — atmospheric pressure, motivation time, and Positive End Expiratory Pressure (PEEP) — with prepare for more controls in the works.
A group from Lehigh University and the University of Arkansas for Medical Sciences looked for the most reliable approaches for administering albuterol by means of ventilator. Credit: Rahul Rajendran
Abassi and Liu anticipate the ventilators helping not simply overloaded health centers in the United States however likewise in establishing nations and backwoods with restricted medical facilities. “If they can build it at home, they can use it,” stated Abassi. “And you can build many of these ventilators in a very short time.”
Patients on ventilators who have some lung conditions pertinent to COVID-19 with underlying persistent lung illness will frequently get drugs like albuterol through an endotracheal tube. This treatment unwinds the bronchial muscles and enhances air flow to the restricted lung respiratory tracts.
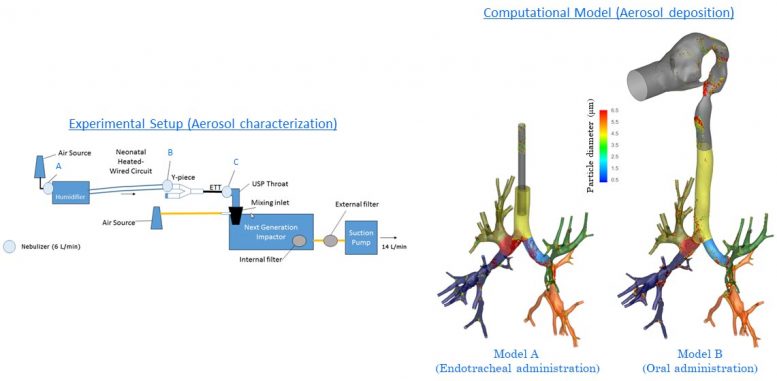
A group from Lehigh University and the University of Arkansas for Medical Sciences looked for the most reliable approaches for administering albuterol by means of ventilator.
Ariel Berlinski and his group carried out aerosol characterization experiments at the University of Arkansas. Rahul Rajendran at Lehigh utilized the outcomes to examine drug shipment through calculations.
“The research objective was to evaluate the efficiency of drug delivery when the nebulizer type and its placement were varied in the ventilator circuit,” stated Arindam Banerjee, a member of the group and a Lehigh teacher of mechanical engineering and mechanics.
The scientists discovered that a vibrating mesh (instead of a jet) nebulizer put on the dry side of the humidifier provides the greatest dosage to the lung. Administering albuterol through intubation works most efficiently for smaller sized particles, while oral administration is more effective for bigger particles.
“Our results are vital for mechanical ventilator based treatment,” stated Banerjee.
Even in ideal scenarios, health care employees still run the risk of contracting COVID-19. A brand-new breathing device might lower breathed out aerosols, which are understood to transfer the infection that triggers the illness.
Researchers from Liberty University and Vapotherm questioned how typical breathing treatments would impact aerosol emissions. So they chose to evaluate a proposed style for a PVC face mask linked to suction, including a high-velocity nasal insufflation cannula — the type of tubed gadget that provides oxygen to the nose.
Then, with input from medical specialists, they designed a health center space with 2 clients and 4 caretakers utilizing extremely advanced computational strategies. According to their design, when clients use the brand-new device, less particles reach the health care employees.
“It represents an inexpensive way to reduce the spread of airborne contagion using supplies commonly found in hospital rooms already,” stated engineering PhD prospect Reid Prichard. “This will remain an important tool even after the pandemic is over.”
Another group from the University of South Florida, led by mechanical engineering PhD trainee Anthony Perez, is examining what occurs to any aerosol impurities that clients do release into a health center seclusion space — and how rapidly the impurities leave the space.
“As lots of health centers are reaching capability, guaranteeing a health center space is safe to get in after an aerosol-generating treatment — or after the elimination of a previous client so hygiene employees can prepare the space — needs considerable down time,” stated Perez.
According to the scientists, the Centers for Disease Control and Prevention ventilation suggestions presume pathogen-containing aerosols are completely blended within a space. Using mathematical simulations, the group discovers that imperfect mixing conditions considerably impact how rapidly ventilation gets rid of pathogens from a space.
“It is both surprising and somewhat concerning that the standard for air sanitization is based on what many would consider a back-of-an-envelope calculation,” stated Perez.
The simulations recommend aerosol impurities can stick around in “dead zones” for around 10 minutes in a normal healthcare facility seclusion space. Meanwhile, “short circuits” expel some packages of impurities rapidly prior to they can distribute.
“Our research illustrates the need for a more accurate, yet inexpensive, framework for the prediction of aerosol concentrations in an arbitrary hospital room, especially in assessing the level of exposure of healthcare workers,” stated Perez.
References:
Design, Build and Test of an In-House Made Ventilator System
Albuterol Delivery Through An Adult Ventilator Circuit To A Patient-Specific Tracheobronchial Airway Model
Novel Use of a Common Respiratory Treatment: Diminishing COVID-19 Transmission
Numerical Investigation of the Role of Air Ventilation Rate in Reducing Healthcare Worker Exposure to Infectious Aerosols in a Hospital Isolation Room





